Chemicals are a part of so many products, and those produced for healthcare environments are no different. Of the more than 4,000 environmental chemicals that have been identified as contact allergens, rubber glove chemicals are among the most frequent causes of allergic contact dermatitis (ACD) in healthcare workers. According to the CDC, contact dermatitis is one of the most common types of on-the-job illnesses, with treatment costs exceeding $1 billion annually.
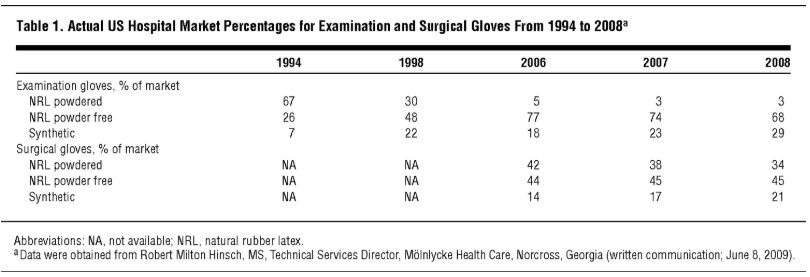
Most people associate rubber glove allergies with latex, but non-latex gloves can cause allergic reactions as well. While the healthcare industry has moved away from latex over the past decade (See Table 1), skin allergies to non-latex gloves have increased. The reactions have been mostly characterized as chemical or Type-IV allergies.
Type-IV allergies are typically attributed to Sulphur-based chemical accelerators (predominantly thiazoles, thiurams and carbamates) that are used to ensure a rapid vulcanization of the polymers in nitrile or other non-latex exam gloves. For some, exposure to these chemicals can result in reddening, itching or burning of the skin, potentially impacting the ability to safely care for patients.
To provide the safest environment possible for staff, those responsible for purchasing products for their healthcare facility need to be up-to-date and informed about the product allergenic risks and ensure needed alternatives are on hand. In addition to reducing allergy-related suffering for thousands of healthcare workers, making this a priority among allergy management programs makes good business sense as well, as the aftermath of these reactions can potentially represent increased costs for hospitals in missed shifts and corresponding staffing challenges.
Related Article
Here are a few things to consider when putting policies and products in place to mitigate the risk for these allergies in your facility:
 What are the trade-offs? The chemicals in question help to ensure a rapid vulcanization of the polymers in the glove and are typically responsible for many of the beneficial characteristics, such as strength, elasticity and barrier performance. While historically it’s been difficult to have these same benefits while avoiding the potentially allergenic chemicals that made them possible, ongoing focus on this issue and new advances in formulations and processes have changed that in recent years.
What are the trade-offs? The chemicals in question help to ensure a rapid vulcanization of the polymers in the glove and are typically responsible for many of the beneficial characteristics, such as strength, elasticity and barrier performance. While historically it’s been difficult to have these same benefits while avoiding the potentially allergenic chemicals that made them possible, ongoing focus on this issue and new advances in formulations and processes have changed that in recent years.- Ensuring consistency and performance. Be sure to talk with your vendor about the options currently available to you to help mitigate risks and best protect those in your current workforce with known allergies. How do their offerings hold up against ASTM and other standards? Are there certain applications or care settings where they cannot be used (such as in chemotherapy delivery)? How have they considered clinician comfort and fit? These are all things you should be asking and your vendor should be prepared to discuss.
- Reassess your product mix and needs frequently. According to a recent report, the hospital staff turnover rate nationally stands at 19.1% and turnover among nursing staff in particular is increasing. With these changes comes a need to keep an open line of communication between unit managers and supply chain professionals to ensure what is currently on hand best protects the needs of the staff—current and future.
While hospitals are patient-centric organizations, the protection of the staff responsible for the care of those patients is critical as well. Commonly used personal protective equipment like gloves are an important piece of that puzzle. However, if the chemicals used in the production of that glove can trigger an allergic reaction, there’s the potential for more harm than good—both for the individual wearing them and the organization as a whole.
 What are the trade-offs? The chemicals in question help to ensure a rapid vulcanization of the polymers in the glove and are typically responsible for many of the beneficial characteristics, such as strength, elasticity and barrier performance. While historically it’s been difficult to have these same benefits while avoiding the potentially allergenic chemicals that made them possible, ongoing focus on this issue and new advances in formulations and processes have changed that in recent years.
What are the trade-offs? The chemicals in question help to ensure a rapid vulcanization of the polymers in the glove and are typically responsible for many of the beneficial characteristics, such as strength, elasticity and barrier performance. While historically it’s been difficult to have these same benefits while avoiding the potentially allergenic chemicals that made them possible, ongoing focus on this issue and new advances in formulations and processes have changed that in recent years.